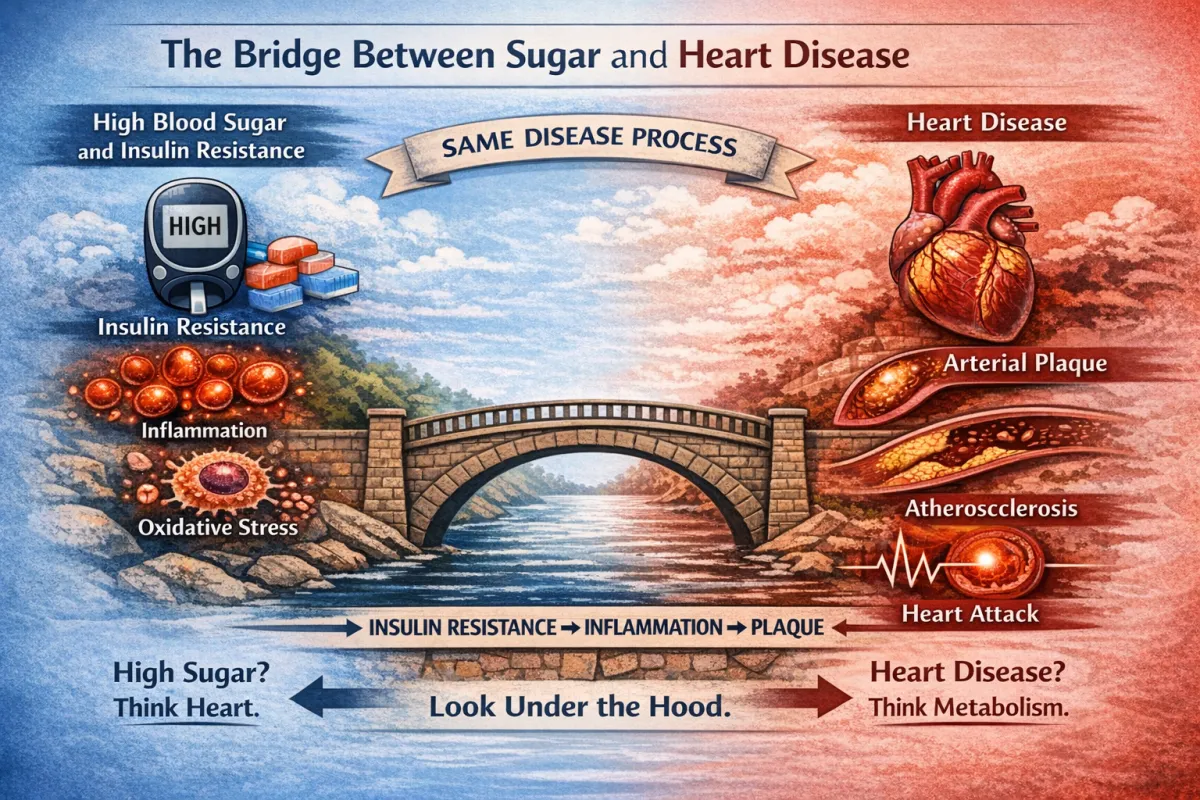
The Bridge Between Sugar and Heart Disease: What Most People—and Most Doctors—Are Missing
The Bridge Between Sugar and Heart Disease: What Most People—and Most Doctors—Are Missing
"Diabetes is a Cardiovascular Disease" ... "Heart Disease Rarely Exists Without Insulin Resistance"
By Dr John Sciales
CardioCore Metabolic Wellness Center
Introduction: Two Diseases… or One?
Most people think of heart disease and diabetes as two completely different problems. Heart disease is associated with cholesterol, blocked arteries, and heart attacks, while diabetes is seen as a condition of elevated blood sugar. They are taught separately, treated separately, and often managed by different specialists.
But what if they are not separate at all?
What if they are two expressions of the same underlying disease process?
This concept is supported by decades of research showing that metabolic dysfunction, particularly insulin resistance, plays a central role in both diabetes and cardiovascular disease [1–3].
Once we understand this, it becomes clear that what we call “sugar” is not the root problem. It is simply the most visible signal of a deeper metabolic issue.
The Limits of a Number-Based Model
Modern medicine relies heavily on numbers, glucose, hemoglobin A1c, LDL cholesterol. These markers are useful, but they often reflect disease late in its course.
For example, diagnostic thresholds for diabetes are based largely on the risk of developing microvascular complications such as diabetic eye disease, not cardiovascular disease, which is the leading cause of death in these patients [4].
Similarly, heart disease is often diagnosed when blockages are advanced enough to affect blood flow, even though atherosclerosis begins years earlier within the vessel wall [5]. Stress testing picks up blockages when they reach >70% and don't identify earlier disease. Yet, >2/3 of all Heart Attacks occur from blockages less than 50% due to unstable plaque and plaque rupture.
This creates a reactive system, one that identifies disease after it has already progressed. Early detection and prevention is not what is rewarded in Corporate medicine: disease and procedures pay the bills.
Sugar Is Not the Disease—It’s the Signal
Blood sugar rises when the body can no longer compensate for metabolic dysfunction. But the process begins much earlier with insulin resistance.
In insulin resistance, the body’s cells do not respond properly to insulin, leading to impaired glucose uptake. To compensate, the pancreas produces more insulin, resulting in hyperinsulinemia [6].
This compensation can maintain normal glucose levels for years, masking the underlying problem.
The Silent Phase of Disease
This early phase, characterized by elevated insulin but normal glucose, can persist for 10–20 years [6,7]. During this time, individuals may appear metabolically “normal” on routine testing. The labs may appear fine but the arteries are starting to feel the pain.
However, studies using oral glucose tolerance testing with insulin measurements have shown that insulin resistance is often present long before glucose abnormalities are detected [7,8]. Everyone knows their sugar level, Hemoglobin A1c and Cholesterol levels, but how many have has their insulin level checked? This is the most sensitive clinical test in detecting early Insulin resistance yet is rarely done.
This silent phase represents a critical window where intervention could prevent progression, but it is rarely identified in standard clinical practice.
"If you don't look, you don't find... yet it is clear as day".
From Insulin Resistance to Inflammation
Insulin resistance is not just a metabolic problem, it is also an inflammatory one.
Elevated insulin levels activate intracellular pathways such as MAP kinase signaling, which promote inflammation, oxidative stress, and endothelial dysfunction [9]. At the same time, insulin resistance is associated with activation of the NF-κB pathway, a key regulator of inflammatory gene expression [10].
Chronic low-grade inflammation is now recognized as a central mechanism linking metabolic dysfunction to cardiovascular disease [2,11]. Yet therapies aimed at lowering blood glucose do not uniformly suppress inflammatory signaling, particularly at the level of NF-κB. In fact, reductions in glucose or hemoglobin A1c are not reliably associated with reductions in inflammatory burden. Glucose is a late and relatively weak marker of the underlying biology.
It does not reflect the chronic inflammatory and metabolic stress that drives atherosclerosis. When we focus solely on glucose, we risk treating the number while missing the disease.
"Glucose tells us where we are. Inflammation tells us what has been happening for years".
The Vascular Connection
The endothelium, which lines the blood vessels, plays a critical role in maintaining vascular health. It regulates blood flow, prevents clotting, and controls inflammatory responses.
In insulin resistance, endothelial function becomes impaired. Nitric oxide production decreases, leading to reduced vasodilation and increased vascular stiffness [12].
This condition, known as endothelial dysfunction, is one of the earliest detectable abnormalities in atherosclerosis and predicts future cardiovascular events [12,13].
Plaque as a Biological Response
Atherosclerosis is often described as a buildup of cholesterol in the arteries. However, this is an oversimplification.
Plaque formation is a complex biological process driven by inflammation, immune activation, and metabolic dysfunction. Cholesterol plays a role, but it is part of a larger inflammatory response within the vessel wall [11,14].
As Libby and colleagues have demonstrated, atherosclerosis is fundamentally an inflammatory disease [11].
From this perspective, plaque represents the structural consequence of years of metabolic injury.
Heart Disease Begins Earlier Than We Think
By the time plaque is visible on imaging, the disease process is already well established.
Importantly, many individuals with coronary artery disease do not meet traditional criteria for diabetes. Studies have shown that when more sensitive testing is used, a large proportion of these patients have underlying abnormalities in glucose metabolism [15].
In 2013 the American Journal of Cardiology has demonstrated the vast majority of patients (88%) with a heart attack but normal sugars will have an abnormal Oral Glucose Tolerance Test, yet I have never seen a cardiologist order it[15]. Unfortunately they don't know what to do with the information. This is a major problem with today's cardiovascular risk reduction strategies. In a way cardiology excels in LDL reduction and not total CV risk reduction.
"This highlights the limitations of relying solely on fasting glucose or A1c"
The Misleading Comfort of “Normal”
A “normal” lab result does not always mean normal physiology.
Insulin resistance, hyperinsulinemia, and early vascular changes can all be present in individuals with normal glucose and cholesterol levels. Normal Stress Tests do not mean Normal arteries.
This disconnect helps explain why many patients experience cardiovascular events despite having “controlled” risk factors. A “sudden” cardiovascular event is almost never sudden. It represents years of silent disease progression that was simply not identified. The real issue is not unpredictability, it is under-detection. Not looking, when the tools exist, is the true sin of omission.
Large trials such as COURAGE and ISCHEMIA have shown that treating flow-limiting lesions alone does not necessarily reduce major cardiovascular events, emphasizing that the disease extends beyond obstruction [16,17].
Reframing the Disease Process
When viewed through a metabolic lens, the progression becomes clear:
Insulin resistance leads to compensatory hyperinsulinemia or elevated insulin levels, which drives inflammation and endothelial dysfunction. Over time, this results in plaque formation and cardiovascular disease.
Glucose elevation occurs later, signaling that the system has reached a point where compensation is no longer sufficient.
"This explains why diabetes is considered a cardiovascular disease equivalent, with similar risk for future events [18]"
A Functional Medicine Perspective
Functional medicine focuses on identifying and addressing the root causes of disease. We don't wait until disease happens and we prioritize wellness.
Rather than treating isolated numbers, it evaluates the broader metabolic environment, including nutrition, physical activity, sleep, stress, and gut health.
Each of these factors influences insulin sensitivity and inflammation, and together they shape long-term health outcomes [19].
This approach aligns with growing evidence that lifestyle interventions can significantly improve metabolic health and reduce cardiovascular risk [20].
Looking Under the Hood
To truly understand disease risk, we must go beyond standard testing.
Advanced metabolic testing, including insulin measurements during an oral glucose tolerance test, can detect early insulin resistance [7].
Imaging tools such as coronary artery calcium (CAC) scoring and coronary CT angiography (CCTA) provide direct assessment of atherosclerotic burden and plaque characteristics [21,22]. Stress Testing misses these.
These tools allow us to identify disease earlier and tailor interventions more effectively.
The Importance of Early Detection
Early detection changes everything.
When metabolic dysfunction is identified early, we have the opportunity to improve insulin sensitivity, reduce inflammation, and change the course of disease. But diabetes does not exist in isolation, the choice of therapy is fundamentally linked to the presence or absence of cardiovascular disease, as reflected in American Diabetes Association recommendations. If you do not look for heart disease, you are not practicing precision medicine. You are treating diabetes blindly.
This represents a shift from reactive to proactive care, one that focuses on prevention rather than late-stage treatment.
Heart disease and diabetes are inseparable expressions of the same underlying biology. To treat one without actively looking for the other is to practice incomplete medicine.
"Yet this is exactly what happens every day in clinical care"
Conclusion: A New Way of Seeing
The connection between sugar and heart disease is not a coincidence. It is the result of a shared underlying process driven by metabolic dysfunction.
Blood sugar is not the beginning of disease, it is a late marker of a process that has been unfolding for years.
By shifting our focus from numbers to biology, we can better understand, detect, and treat disease at its root.
Call to Action
If you have been told your labs are normal but still have concerns about your health, it may be time to look deeper. Labs are designed to reveal disease rather than identifying risk before it occurs. That is Reactive... Here at CardioCore we are ProActive in identifying risk and using natural ways to optimize Health.
We combine advanced testing including Genetic, Hormonal, Metabolic and Gut microbiome analysis to uncover what traditional evaluations often miss. Through nutrition, targeted supplements, exercise, sleep optimization, stress reduction, socialization, spirituality, and gut microbiome support, we design personalized prevention strategies centered on the whole person. We specialize in creating wellness outcomes, not merely treating disease.
We understand the Inflammatory drivers of both Diabetes and Heart Disease and we use Holistic and Natural ways to Optimize your Health and Wellness.
Stop guessing. Start seeing.
Book a Call and Find Out More... Dr John
CLICK HERE TO BOOK A DISCOVERY CALL
CLICK HERE TO JOIN OUR PRIVATE CardioCore COMMUNITY
CLICK HERE TO SPEAK TO OUR VIRTUAL ASSISTANT
This article is dedicated to Lillian, who has diabetes and Coronary artery disease. She is not being treated as per the established Standards of Medical Care by her Cardiologist, Endocrinologist and Primary Care Physician. One questions why, not one, but all three of her doctors don't understand or pay attention to the link between the two; Siamese twins in this scenario is the rule, not the exception. Heart disease and Insulin Resistance will be forever linked. Ignoring this has serious consequences regarding her Cardiovascular risk reduction strategies and ultimately her longevity.
References
Reaven GM. Banting Lecture: Role of insulin resistance. Diabetes. 1988.
DeFronzo RA. Pathogenesis of type 2 diabetes mellitus. Med Clin North Am. 2004.
Grundy SM. Metabolic syndrome and cardiovascular disease. Circulation. 2005.
ADA. Standards of Medical Care in Diabetes. Diabetes Care.
Glagov S, et al. Compensatory enlargement of atherosclerotic arteries. N Engl J Med. 1987.
Shanik MH, et al. Insulin resistance and hyperinsulinemia. Diabetes Care. 2008.
Abdul-Ghani MA, et al. Early detection of insulin resistance. J Clin Endocrinol Metab. 2006.
Tabák AG, et al. Prediabetes progression. Lancet. 2012.
Muniyappa R, et al. Insulin resistance and endothelial dysfunction. Endocr Rev. 2007.
Shoelson SE, et al. Inflammation and insulin resistance. J Clin Invest. 2006.
Libby P. Inflammation in atherosclerosis. Nature. 2002.
Bonetti PO, et al. Endothelial dysfunction. Circulation. 2003.
Vita JA. Endothelial function and cardiovascular risk. Circulation. 2011.
Hansson GK. Immune mechanisms in atherosclerosis. Nat Rev Immunol. 2005.
Norhammar A, et al. Glucose metabolism in CAD. Eur Heart J. 2002.
Boden WE, et al. COURAGE trial. N Engl J Med. 2007.
Maron DJ, et al. ISCHEMIA trial. N Engl J Med. 2020.
Haffner SM, et al. Diabetes as CAD equivalent. N Engl J Med. 1998.
Mechanick JI, et al. Lifestyle medicine. Endocr Pract. 2020.
Knowler WC, et al. Diabetes Prevention Program. N Engl J Med. 2002.
Budoff MJ, et al. Coronary calcium guidelines. JACC.
SCOT-HEART Investigators. CCTA outcomes. Lancet.
