High Blood Pressure Unmasked: Why Metabolic Dysfunction—Not Just Your Heart—is the Real Culprit
High Blood Pressure Unmasked: Why Metabolic Dysfunction—Not Just Your Heart—is the Real Culprit
Most patients with elevated blood pressure are sent straight to the cardiologist. After all, hypertension sounds like a “cardio” problem. But here’s the shocking truth:
High blood pressure is not simply the result of cardiovascular dysfunction. It is the downstream effect of metabolic dysfunction.
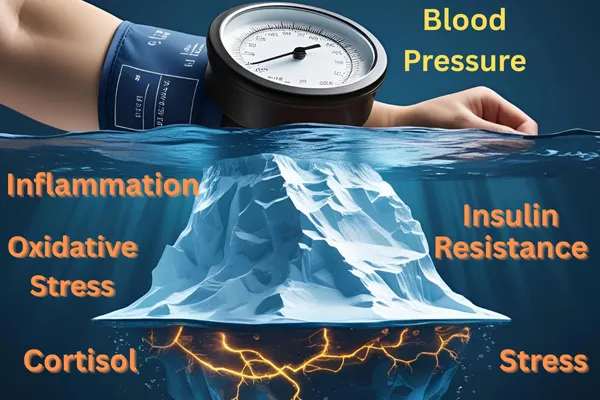
Your heart is often just the first visible victim of a much deeper problem. The true engine of hypertension is insulin resistance—a metabolic breakdown that drives fluid retention, artery stiffening, hormone imbalance, inflammation, and nervous system overdrive.
When doctors treat hypertension as if it were purely a cardiac issue, they’re chasing sparks while ignoring the raging fire underneath.
Insulin Resistance: The Hidden Engine of Hypertension
Insulin is the hormone that moves glucose (sugar) from your blood into your cells to be used for energy. But when your cells stop responding properly—a state called insulin resistance—your body compensates by pumping out more insulin.
This chronic flood of insulin (hyperinsulinemia) doesn’t just set the stage for diabetes. It is one of the most powerful, overlooked drivers of high blood pressure.
And here’s the kicker: I’m almost certain your cardiologist never checked your fasting insulin level or your insulin response to a glucose challenge. Yet these tests are far more predictive of cardiovascular and cardiometabolic risk than cholesterol or even blood pressure itself [1,2].
Here’s how insulin resistance drives hypertension through five major mechanisms:
Sodium Retention
High insulin tells your kidneys to hold onto sodium and water. This expanded fluid volume raises blood pressure—like overfilling a balloon [3].RAAS Activation (Renin–Angiotensin–Aldosterone System: your body’s hormone system for blood pressure)
Insulin resistance overstimulates RAAS, producing excess angiotensin II (a vessel constrictor) and aldosterone (which locks in sodium and water). Together, they squeeze arteries and drive pressure higher [4].Endothelial Dysfunction (Damaged Vessel Lining)
The endothelium, the inner lining of blood vessels, normally produces nitric oxide (NO), a natural vessel relaxer. Insulin resistance suppresses NO, leaving arteries stiff and constricted [5].Overactive Sympathetic Nervous System (“Fight-or-Flight” Mode)
Insulin resistance overstimulates the sympathetic nerves, leading to faster heart rate, stronger contractions, and tighter arteries—all fueling hypertension [6].Chronic Inflammation & Hormonal Chaos
Insulin resistance creates low-grade inflammation. This raises stress hormones like cortisol and boosts aldosterone, amplifying sodium retention and vascular constriction [7].
The result? Blood pressure climbs—not because your heart is failing, but because your metabolism is inflamed and overloaded.
Why Drugs Alone Miss the Point
Most doctors are trained to treat hypertension as a number problem. Too high? Prescribe a pill. But not all blood pressure medications are equal, and lowering blood pressure does not always translate into the same reduction in cardiovascular risk [8,9].
Diuretics (“water pills”) lower pressure by dumping salt and water, but often worsen glucose control and raise uric acid.
Beta blockers (atenolol, metoprolol, propranolol) are poor antihypertensives. They may reduce heart rate but often worsen insulin resistance and metabolic dysfunction [10].
Calcium channel blockers (like amlodipine) relax arteries and can lower blood pressure effectively. But here’s the critical point: their BP-lowering effect is not as strongly linked to reduced cardiovascular events as one would expect [8,9]. Amlodipine reduces the cuff number but leaves insulin resistance, RAAS overdrive, and inflammation largely untouched. Importantly, unlike ACE/ARB drugs, amlodipine provides no meaningful renal protection. It lowers blood pressure, but it does not slow kidney damage, which is tightly linked to hypertension and metabolic dysfunction.
ACE inhibitors & ARBs (lisinopril, ramipril, losartan, valsartan) go much deeper. By blocking RAAS, they lower blood pressure, improve insulin sensitivity, protect the blood vessels, and protect the kidneys. Landmark trials in patients with diabetes and proteinuria showed that ACE/ARB therapy slowed kidney decline and reduced cardiovascular events [11,12].
The lesson? Two patients can both drop their blood pressure by 10 points—one on amlodipine, the other on lisinopril—but the lisinopril patient gains protection for the heart, blood vessels, and kidneys. Mechanism matters more than the number.
The Bigger Picture: Cardiometabolic Health
High blood pressure is rarely an isolated condition. It is part of the modern epidemic of cardiometabolic disease, which includes:
Cardiovascular disease: heart attacks, strokes, atherosclerosis
Type 2 diabetes: driven by chronic insulin resistance
Metabolic syndrome: abdominal obesity, high triglycerides, low HDL, and hypertension
Nonalcoholic fatty liver disease (NAFLD): fat buildup in the liver
Dementia & Alzheimer’s disease: increasingly called “type 3 diabetes”
All of these share the same foundation: insulin resistance, oxidative stress, and inflammation [13].
This is why treating blood pressure metabolically doesn’t just lower the cuff reading—it protects your whole body.
At this point, traditional medicine often stops. It celebrates the lower number on the blood pressure cuff. But at CardioCore Metabolic Wellness Center, we ask the harder question: Did we actually change the disease process itself?
Our mission is simple but powerful:
“Getting to the Core… the Path to Wellness – where being Healthy is not an Accident.”
We don’t just chase numbers. We uncover the root causes—insulin resistance, inflammation, and early plaque formation—long before disaster strikes. That’s why our approach includes:
✅ Advanced testing for insulin resistance and metabolic drivers of disease
✅ CT calcium scoring and vascular imaging to identify risk early
✅ Nutrition strategies centered on whole foods, healthy fats, and carb control
✅ Lifestyle and supplement protocols that target inflammation and restore vascular health
✅ Personalized prevention plans that protect the heart, brain, kidneys, and metabolism
This isn’t about masking symptoms. It’s about rewriting the trajectory of your health.
Conclusion: Stop Chasing Numbers, Start Treating the Core
High blood pressure is not the result of a failing heart. It is the result of a failing metabolic system. Cardiovascular dysfunction is simply the downstream damage.
When we only target the blood pressure number with drugs, we miss the chance to correct the real disease process. At CardioCore, we put out the fire instead of chasing sparks.
Your health is not an accident. It is the result of choices, environment, and proactive care.
👉 CLICK HERE TO BOOK A DISCOVERY CALL
👉 CLICK HERE TO JOIN OUR PRIVATE CardioCore COMMUNITY
👉 CLICK HERE TO SPEAK TO OUR VIRTUAL ASSISTANT
References
Reaven GM. Role of insulin resistance in human disease. Diabetes. 1988;37(12):1595–1607.
Muniyappa R, Lee S, Chen H, Quon MJ. Current approaches for assessing insulin sensitivity and resistance in vivo. Endocr Rev. 2008;29(6):585–602.
Ferrannini E, Natali A. Essential hypertension, metabolic disorders, and insulin resistance. Am Heart J. 1991;121(4 Pt 2):1274–1282.
Lastra G, Dhuper S, Johnson MS, Sowers JR. Salt, aldosterone, and insulin resistance: impact on the cardiovascular system. Nat Rev Cardiol. 2010;7(10):577–584.
Steinberg HO, et al. Insulin-mediated skeletal muscle vasodilation is nitric oxide dependent. J Clin Invest. 1994;94(3):1172–1179.
Esler M, Rumantir M, Kaye D, Jennings G, Hastings J, Socratous F. Sympathetic nervous system and insulin resistance: a critical review. Hypertension. 2001;37(2):394–398.
Shoelson SE, Herrero L, Naaz A. Obesity, inflammation, and insulin resistance. Gastroenterology. 2007;132(6):2169–2180.
Messerli FH, Bangalore S, Bavishi C, Rimoldi SF. Angiotensin-converting enzyme inhibitors in hypertension: to use or not to use? J Am Coll Cardiol. 2018;71(13):1474–1482.
Psaty BM, et al. Health outcomes associated with antihypertensive therapies used as first-line agents. JAMA. 1997;277(9):739–745.
Bangalore S, Parkar S, Grossman E, Messerli FH. A meta-analysis of beta-blockers for hypertension and cardiovascular disease. Am J Med. 2007;120(8):719–729.
Yusuf S, Sleight P, Pogue J, Bosch J, Davies R, Dagenais G. Effects of an ACE inhibitor, ramipril, on cardiovascular events in high-risk patients. N Engl J Med. 2000;342:145–153.
Brenner BM, Cooper ME, de Zeeuw D, et al. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med. 2001;345:861–869.
Grundy SM. Metabolic syndrome pandemic. Arterioscler Thromb Vasc Biol. 2008;28(4):629–636.
